Gut microbiota info
Microbiota: a definition
Scientists define microbiota as “the assemblage of microorganisms (all the bacteria, archaea, eukaryotes, and viruses) present in a defined environment.” More specifically, the microbiota varies according to its surrounding environment. The term microbiota is thus preceded by the name of the environment in which it is located. For example, ‘gut microbiota’ refers to the microbiota in the intestinal tract.
Microbiome: a definition
The term microbiome was initially used to refer to the collection of genes harbored by microorganisms.
A broad definition of microbiome encompasses “the entire habitat, including the microorganisms (bacteria, archaea, lower and higher eukaryotes, and viruses), their genes, and the surrounding environmental conditions.”
However, to simplify, the term ‘microbiome’ is commonly used to refer to the microorganisms you harbor in and on your body (i.e., your microbiota).

In an individual weighing 70kg, the human gut microbiota gathers more than 100 trillion microorganisms and weighs about 200g (equivalent to a medium-sized mango). There are 150/200 times more genes in this individual’s microbiota than in all of their cells put together.
The human genome consists of about 23,000 genes, whereas our microbiome encodes over 3 million genes that produce thousands of metabolites. In other words, in terms of genes, humans are more than 99% microbial.
Although there is a ‘core’ consisting of bacterial groups common to all healthy humans (it has been estimated that one third of the gut microbiota is common to most people), gut microbiota composition is mostly unique to each individual and is influenced by:
Factors over which humans can take action:
- feeding methods (breast milk, artificial milk and introduction of solid food);
- medication (antibiotics, acid suppressants, anti-diabetic drugs…);
- dietary habits and the way food is cooked;
- environment and lifestyle (rural vs. urban locations, exercise); and
- weight gain.
Factors over which humans cannot take direct action:
- genetics;
- the anatomical part of the intestinal tract (e.g., the large intestine has a higher microbial diversity compared with the small intestine);
- gestational age (preterm birth vs. full-term birth);
- delivery mode (vaginal delivery vs. C-section); and
- aging.
Interestingly, even though each individual has a specific microbiota that acts like an individual identity card, the microbiota in general also brings unique functions to humans (e.g., digesting nutrients that humans cannot digest on their own and producing vitamins, among others).
Although there is no consensus on what constitutes a health-associated microbiota, some hallmarks have been proposed:
- Increased species richness and/or diversity: the number of different species and how different they are in a specific habitat (e.g., the digestive tract) is considered a hallmark of gut health.
- Resistance, resilience and stability over time: the ability to resist perturbation (e.g., antibiotic treatment or imbalanced diets) and to recover a stable state.
- High gut microbial gene richness: the number of microbial genes in the gut has been suggested as an indicator of good metabolic and overall health.
Digestive ailments, obesity, diabetes, allergies, cancer and even neurodegenerative diseases have been linked to an imbalance in gut microbiota composition or function (a situation scientists call ‘dysbiosis’).
Thus, targeting the gut microbiota emerges as a potential way of dealing with many chronic diseases that are on the rise in Western society.
Microbes were here before humans arrived. The intestine is considered one of the most densely populated microbial habitats known on earth. In humans, other microbes can also be found in the nose, mouth and throat, small intestine, lungs, vagina, and skin.
Gut microbiota functions are manifold:
Defense:
- It defends against harmful microorganisms.
- It teaches the immune system to tell friends from foes.
- It degrades toxic compounds.
Nutrition:
- It can digest certain foods (e.g., dietary fiber) that humans are not able to digest.
- When the gut microbiota breaks down dietary fiber, it produces important molecules (e.g., short-chain fatty acids) with benefits that go beyond the gut.
- It facilitates absorption of dietary minerals (e.g., magnesium, calcium and iron).
- It synthesizes some essential vitamins (e.g., vitamin K and folate (B9)) and amino acids (i.e., the building blocks of proteins).
Behavior:
- It can shape mood and behavior.
Given its important functions, scientists nowadays consider the gut microbiota to be an ‘organ’.
Colonization of the gut by the human microbiome was thought to begin at birth, but some scientists have reported that a mother-to-child transfer of commensal bacteria through the placental barrier may occur. The maternal oral microbiome has been suggested as the source of the first bacteria that colonize infants.
Delivery mode has a major influence on the gut microbiota in early life. When born vaginally, an infant is colonized by the mother’s gut and vaginal microbiota first. In contrast, when the baby is delivered via Caesarean section, it is exposed to the skin and hospital environment microbiota first. Recent data also suggests rectal mother-to-child bacterial transmission.
As such, in early life, the infant born vaginally acquires bacteria resembling its own mother’s vaginal and fecal microbiota, showing a low level of diversity and depending mainly on the baby’s diet.
Afterwards, mode of feeding—breast milk versus formula—has a major impact on the composition of the infant’s microbiota. Human breast milk not only contains live bacteria, but also a great variety of complex carbohydrates (named human milk oligosaccharides) that cannot be digested by babies. In turn, these complex carbohydrates act as prebiotics by influencing the composition of the bacteria in the infant’s gut. While the gut microbiota of breastfed infants is dominated by Lactobacillus and Bifidobacterium, formula-fed infants develop a microbiota resembling that of an adult, with higher overall bacterial diversity.
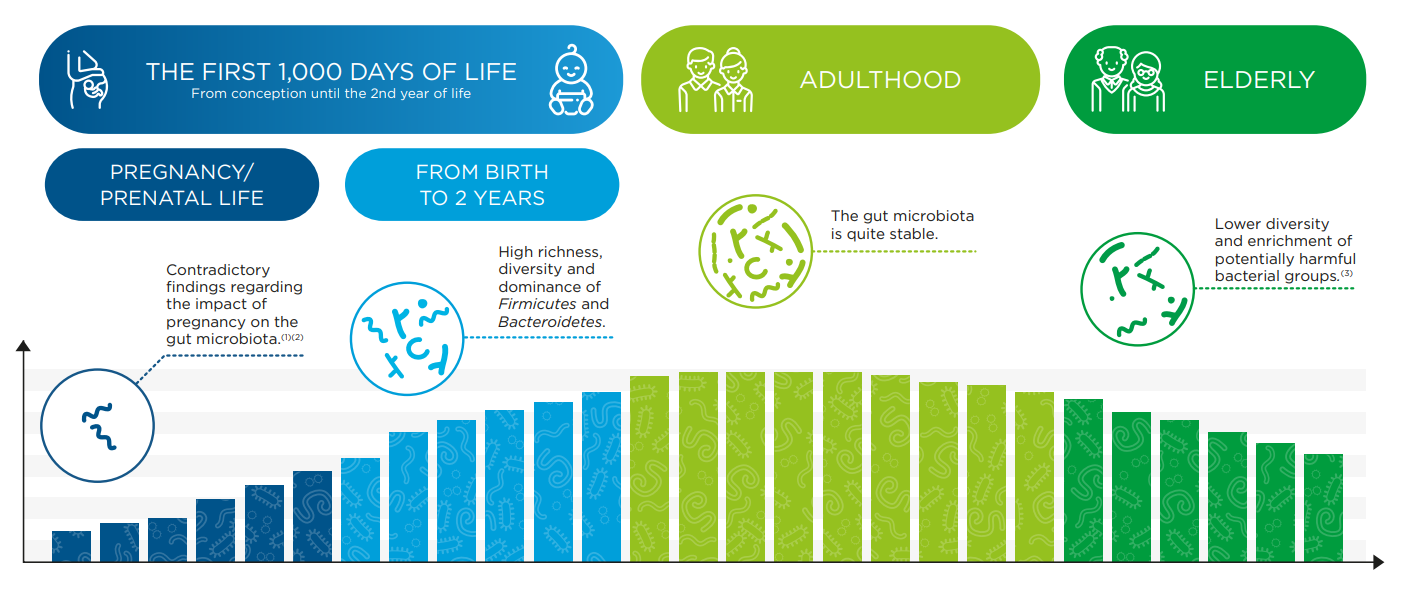
The transition from breastfeeding to solid foods high in protein and fiber leads to an increase in gut bacteria diversity. Scientists consider that by the time a child is between 2 and 3 years old, their gut microbiota resembles that of an adult and will remain stable during their adult life.
Changes occur throughout life in the gut microbiota, from infancy to old age. While the gut microbiota is highly variable in newborns, as humans age, it tends to remain relatively stable and is accompanied by a lower level of diversity and a loss of important genes such as those involved in producing short-chain fatty acids. This overall decrease in gut microbiota diversity has been tied to increased frailty.
The good news is that these age-related changes in the gut microbiota are partly avoidable through lifestyle. This means that looking after your gut microbiota through a healthy diet and active lifestyle is the best recipe for enjoying good health and well-being.
Both prebiotics and probiotics may help keep your gut microbial lawn healthy.
- Prebiotics available naturally in some foods (e.g. chicory root, vegetables and whole grains) and food supplements can be selectively utilized by your microorganisms, conferring a health benefit.
While you can’t digest fibers and prebiotics, certain beneficial microbes can. Some fibers are utilized by gut microbes, but this is not a requirement for fiber. By contrast, prebiotics are selectively utilized by resident microbes.
- Probiotics are live microorganisms that, when administered in sufficient amounts, confer a health benefit on the host. Certain fermented foods such as yogurt can help (or participate in maintaining) your gut microbiota, so as to ensure its balance, integrity and diversity by contributing living beneficial bacteria and a wealth of important compounds produced during fermentation.
- In humans, there are about as many bacterial cells as there are human cells. But bacteria have 150 to 200 times more genes than the human genome.
- Gut microbiota richness, diversity and stability over time are key features of a health-associated human gut microbiome.
- Your gut is more than a tube. It’s home to more than 100,000 trillion microorganisms that participate in the digestion and defense functions of the gastrointestinal tract. They could also be involved in mental health.
- Like your fingerprint, your gut microbiota composition is unique to each individual.
- External factors can affect your gut microbiota. While some are less controllable (e.g. genetics, delivery methods, geography and aging), you can act on your diet and lifestyle to help your gut microbiota work properly.
- What you eat doesn’t only nourish you; it also feeds the trillions of microorganisms that live in your gut. Include prebiotic fibers and fermented foods with probiotics, as you make progress on the path towards a healthy gut.